Before you start pumping read on….
An Insulin Pump is another way of delivering insulin rather than using a syringe or pen. It is a small programmable battery-powered device that is worn externally on the body. An insulin pump contains a syringe of insulin which is changed by the user every 2-3 days. The syringe of insulin is placed into the pump and it is attached to the body via a narrow tube (infusion set) and a small plastic cannuale that is placed under the skin. Insulin injections are not required by the pump user except for a situation where the pump is not working.
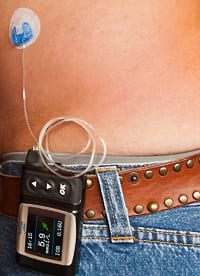 The pump weights approx 3 ozs and measures 7 cms X 5 cms and is usually worn on a belt or carried in a pocket. It is the same size as a pager and is worn in a similar manner.
The pump weights approx 3 ozs and measures 7 cms X 5 cms and is usually worn on a belt or carried in a pocket. It is the same size as a pager and is worn in a similar manner.
Who uses a Pump?
Insulin pump therapy has become popular as part of diabetes management in recent years and there are advantages and disadvantages to it. If you would like more information on insulin pumps speak to your diabetes team. In general, the pump is recommended as an option for people with Type 1 diabetes who, despite multiple daily injection therapy have not been able to maintain a A1c level without experiencing repeated and unpredictable episodes of hypoglycaemia. The sensors would only be sanctioned based on clinical need e.g repeated and unpredictable episodes of hypoglycaemia.
How the pump works
The pump delivers fast acting insulin at a pre-determined, pre-set hourly rate (called a basal rate) and insulin can also be delivered by the user when eating or to correct a high blood sugar (bolus of insulin).
The basal rate of insulin can be set at several different rates over a 24 hour period, depending on the person’s insulin requirements. There is a temporary basal rate function which can be set at a reduced or an increased rate for a precise period of time to allow for exercise or times of illness.
Insulin pumps are a very precise way of delivering insulin as a fraction of a unit of insulin can be delivered reducing the risk of hypoglycaemia.
Before you start using a Pump
Ideally a person on a pump should be carbohydrate counting so they can give a precise amount of insulin for the carbohydrate they are eating. Also each person has an individual ‘insulin sensitivity’ i.e. they know the effect that 1 unit of insulin has on their blood sugar. In that way they can take a precise ‘correction bolus’ of insulin to bring their blood sugar back to the target range they want.
Important facts to consider before you start using a Pump;-
- You will be attached to the pump continuously, it can only be removed for up to 1 hour.
- Only fast acting insulin is used in the pump.
- There is an increased risk of DKA if action is not taken to correct high blood sugars promptly.
- Frequent blood glucose monitoring is essential to determine dosage and ensure that insulin is delivered.
- The pump does not measure blood glucose levels or determine the insulin dose to be delivered – look at the meters webpages for this information.
- To decide how much insulin is needed, a certain level of technical and numerical skills are required.
- If you wish to use the pump, talk to your diabetes team to see if this method of insulin delivery is suitable for you.
Care & Maintenance
The site where the pump is worn has to be changed by the wearer every 3 days, this is a straightforward procedure.
How to get a Pump
Pumps are available on the Long-Term Illness Scheme by individual application from a consultant. Any special accessories such as belts or protectors will generally not be covered. Visit www.funkypumpers.com site to see a range of accessories.
Insurance for Pumps
The only way to get pumps covered is through house insurance and normally it would be 2% of the stated value. Some house insurance companies do not cover pumps and in this case, we advise you to ring Allianz Insurance at 01 448 4848. Travel insurance does not cover the pump.
Closed Loop Systems
The closed loop is also known as the artificial pancreas. In a closed loop, an insulin pump is linked up with a glucose sensor. The sensor communicates with the pump and when the blood glucose levels go below a certain target, the pump is automatically suspended.
A new pump that delivers both insulin (lowers glucose levels) and glucagon (raises glucose levels) is also being studied in clinical trials at present.
Implantable insulin pumps are available but as yet are not used in Ireland. They are surgically implanted in the abdomen and weigh about 6-8 ozs. They provide a background dose of insulin continuously with extra doses delivered with a remote control unit. They are not currently mentioned in international recommendations for the management of diabetes.
Click here to check about what pumps are available in Ireland


