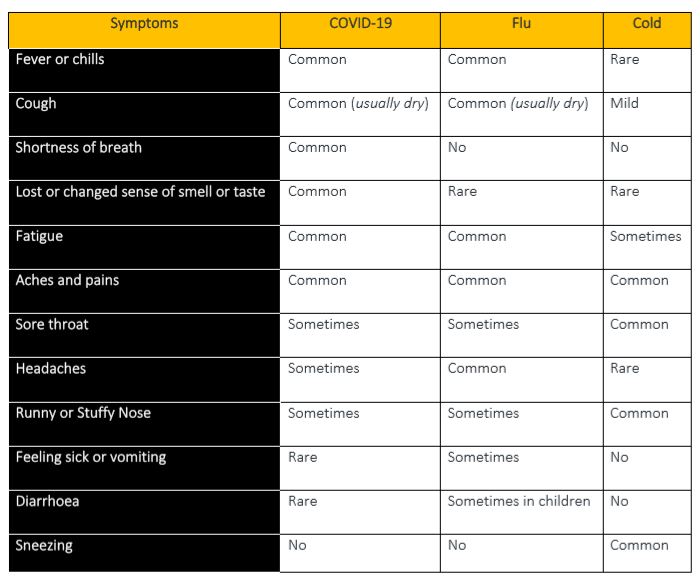
What are the symptoms of COVID-19?
Coronavirus is an umbrella name for virus transmitted to humans from animals. The current strain (COVID-19) is a new variation that until December 2019 was not found in humans.
People with diabetes are considered a high-risk group for COVID 19 because during times of illness or stress the blood glucose levels are higher than normal which makes it more difficult to fight infection. Hence people with diabetes have an increased risk of moderate or severe illness with COVID 19.
The main symptoms to look out for are:
- A cough – this can be any kind of cough, not just dry.
- Shortness of breath.
- Breathing difficulties.
- Loss or change to your sense of smell or taste: this means you’ve noticed you cannot smell or taste anything, or things smell or taste different to normal.
- Fever (temperature above 38 °C or 100.4 °F).
- Other symptoms may include fatigue, headaches, sore throat, aches, and pains.
Do not ignore or delay seeking medical treatment for abnormal signs or symptoms that you may be experiencing.
How can I protect myself from COVID-19
This information is taken from the HSE website.
There are some groups of people who may be more at risk of moderate or serious illness if they get COVID-19.
Diabetes is in the ‘at risk’ group but this does not mean people with diabetes are at higher risk of getting COVID-19, but they are at higher risk of moderate or severe illness.
At-risk groups
You are more at risk of serious illness if you contract COVID-19 and you.
- are 60 years of age and over – people over 70 are particularly vulnerable.
- have a long-term medical condition – for example, heart disease, lung disease, diabetes, cancer, cerebrovascular disease, renal disease, liver disease or high blood pressure.
- have a medical condition that can affect your breathing.
- are a resident of a nursing home or other residential care setting.
- are in specialist disability care and are over 50 years of age or have an underlying health problem.
Extremely vulnerable groups
You are considered extremely vulnerable if you are:
- people aged 70 years or over.
- solid organ transplant recipients.
- people with specific cancers.
- people with severe respiratory conditions including cystic fibrosis, severe asthma and severe COPD.
- people with rare diseases and inborn errors of metabolism that significantly increase the risk of infections (such as SCID, homozygous sickle cell).
- people on immunosuppression therapies sufficient to significantly increase risk of infection.
- women who are pregnant with significant heart disease, congenital or acquired.
How covid 19 is spread
https://www2.hse.ie/conditions/covid19/preventing-the-spread/how-coronavirus-spread/
How to protect yourself and others
https://www2.hse.ie/conditions/covid19/preventing-the-spread/protect-yourself-and-others/
If you have any common symptoms of COVID-19 (coronavirus), self-isolate (stay in your room) and get a COVID-19 test. Other people in your household will need to restrict their movements (stay at home).
To get a free COVID-19 test you can:
- phone a GP
- book a test online
- go to a walk-in test centre
See the following link for public health measures in place right now:
Managing your Diabetes during the COVID pandemic?
It is essential that you put some plans in place to ensure you can look after yourself and your Diabetes in the event of any illness. Maintaining healthy eating practices, looking after your mental as well as your physical health with diabetes is also vitally important.
People with diabetes should prepare themselves so that they are in best possible health and have the necessary knowledge and supplies for when they need to self-treat any illness.
There are simple things you can do today to prepare yourself:
When a person has diabetes, the glucose levels will tend to rise during illness. Therefore, during illness, it is important that you manage your diabetes as well as the illness. Discuss with your diabetes team what to do in the event of illness, they may give you some written instructions to refer to.
- Make sure you have a thermometer – one of the first questions you will be asked if you need to seek medical attention is have you a fever (temperature above 38 °C or 100.4 °F ).
- Ensure you have an adequate supply of non-diet drinks i.e. soft drinks and simple foods that contain some carbohydrate in case you cannot take solid foods.
- Do everything possible to maintain good glucose control.
- Confirm with your diabetes team, what is considered acceptable glucose levels if home testing and when to contact them for assistance.
- For people with Type 1 diabetes, do frequent glucose monitoring and adjust insulin as advised by your diabetes team in accordance with your Sick Day rules management plan. Ensure you have ketone strips.
- If you are using an insulin pump, ensure you have insulins (basal and bolus) to use in case of pump failure.
- For people with Type 2 diabetes – know if you need to alter any medications, during a time of illness. Do contact your GP for medical advice if you are unwell. For general information for people with Type 2 or Prediabetes see Diabetes Smart.
- Make sure you have two weeks supply of medication where possible – ring the pharmacy and arrange date and time for collection the week before your script needs filling. NotePharmacists are to be allowed by law to dispense medicines outside the dates spelled out in prescriptions according to their own professional judgement. In addition, the pharmacist can only dispense one month’s supply of medications per month under the Primary Care Reimbursement Scheme.